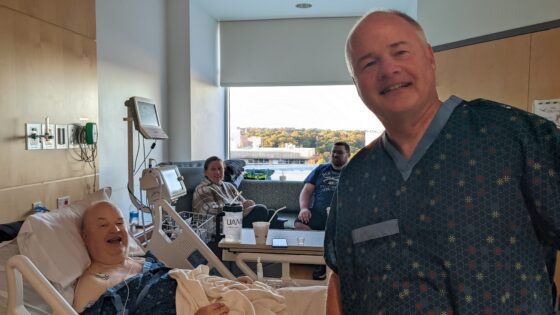
Brotherly Love — UAMS’ Chief Nephrologist Receives Kidney from Younger Sibling
April 26, 2024 | John Arthur, chief kidney doctor at the University of Arkansas Medical Sciences (UAMS), understands the benefits of a living kidney donation more than most people would expect. As the director of the Division of Nephrology in the UAMS Department of Internal Medicine since 2015, he has long been aware that about 100,000 patients across the...